
The healthcare industry is continuing its shift from volume-based care to value-based care, driven in part by changing demands from patients, providers and regulators alike. However, there is still work to be done. While payments are beginning to encourage the proactive management of chronic diseases, some providers are still stuck in the fee-for-service healthcare environment.
Considering the fact that 70% of healthcare costs can be attributed to chronic disease, it’s no surprise that regulators have focused on solutions that address chronic disease management. In fact, the Centers for Medicare & Medicaid Services recently ramped up incentives for Remote Patient Monitoring (RPM) initiatives with the goal of lowering costs of chronic conditions.
Changing the future of RPM and chronic disease
Remote patient monitoring is defined as the use of digital technology, such as connected health devices, to collect patient data and securely send it to healthcare providers. The goal is to help patients manage their diseases - such as type 2 diabetes or heart disease - remotely.
An example of this is our partnership with Companion Medical, in which their smart insulin pen, called InPen, collects insulin dosing data for patients with type 2 diabetes and sends it remotely through an integrated diabetes management app into the Rimidi platform. Working within the electronic health record (EHR), our platform then combines the data provided with additional patient-generated data from smart blood-glucose meters and continuous glucose monitors, as well as relevant clinical data from the EHR to personalize virtual management of the patient. This first-of-its-kind partnership is imperative, as it not only enables innovation in population health and care delivery models, but also results in improving health outcomes. Now, clinicians can analyze real-time insulin dosage data integrated with glucose data to remotely refine dosing decisions, all while working within the existing clinical workflow.
The issue is, however, many healthcare providers have been hesitant to implement RPM due to the limited reimbursement opportunities and lack of incentives for offering such services. But since CMS has recognized the need for change, this should no longer be a challenge.
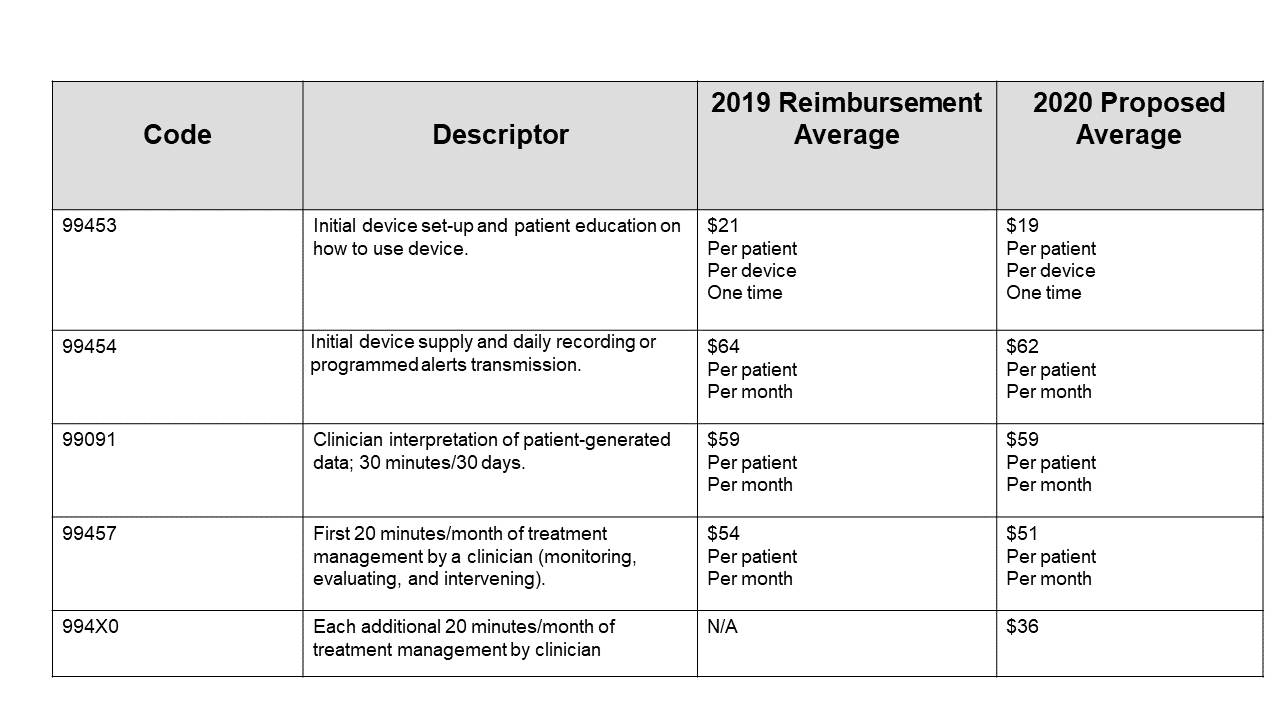
In fact, CMS added three new remote patient monitoring reimbursement codes in 2019 and has recently finalized plans to expand reimbursements in 2020.
If implemented appropriately by healthcare systems, these codes could generate millions of dollars in revenue and also address the confusion around eligibility that has caused pause of RPM implementation by healthcare providers.
Before initiating RPM, providers must obtain patient consent and record it in the EHR. In addition, face-to-face visits are required for new patients or for those who have not seen the billing provider within one year. An annual wellness visit is also required for each patient prior to beginning any RPM program.
Turning RPM data into actionable insights for chronic disease management
To make the most out of your practices RPM initiatives, its crucial to first pick the right technology solution. Consider a solution that:
- Supports multiple chronic disease states
- Creates a continuous feedback loop
- Integrates with your EHR
- Embeds clinical decision-making support
That’s where Rimidi’s platform comes into play. By working seamlessly within the EHR, the platform brings in data from multiple sources and presents it to the clinical team in an easy to understand view. In addition, the platform flags potential concerns, including a concerning change in weight, blood pressure or new medication, to ensure all factors are being taken into consideration when the physician evaluates his or her patient.
More importantly, by integrating such technology into your practice, you’ll experience streamlined workflows, while simultaneously benefitting from more actionable insights and information to enhance patient outcomes.
Remote Patient Monitoring
Rimidi enables practices to effectively run an RPM program-whether your team manages the monitoring or you partner with us for monitoring services.
